Introduction
More than 16 million Americans provide daily help to people with dementia (PWD). Caring for people with disabilities differs from being a family caregiver for several reasons. First, as their physical, cognitive, and emotional abilities deteriorate, PWD requires more caregiver monitoring, dementia support with instrumental activities such as money management or driving, and self-care duties like washing and clothing. Second, PWD behavioural changes and communication challenges may increase caregiving demands and caregiver stress in later phases, leading to losses in caregivers’ mental and physical health.
PWD frequently deal with various chronic diseases and age-related changes, such as diminishing vision and hearing, because age is a critical risk factor for dementia patients. Therefore, a multidisciplinary team must provide continuous, comprehensive, and coordinated treatment for this complex network of functional impairments. Given PWDs’ increasing difficulties with memory and understanding, carers are critical advocates for PWD healthcare to help people with dementia inside and outside clinic visits.
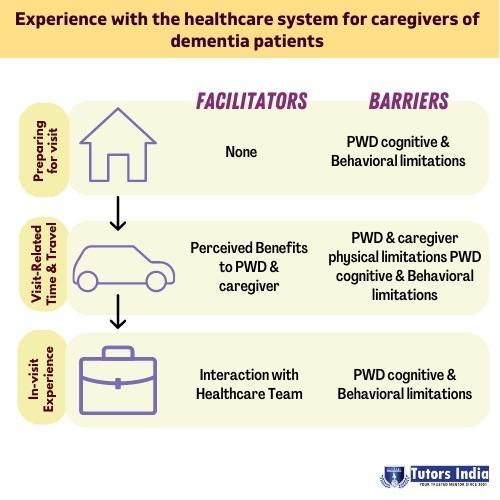
Preparing for visit
The process of mentally and emotionally preparing PWD for a medical appointment is referred to as “preparing for the visit.” The restrictions reported in this group’s caregiver responses were classified as PWD cognitive and behavioural impairments. There was no recognized sub-category for facilitators. The caregivers’ explanations of perceived difficulties are included below, along with, when applicable, facilitation techniques for removing obstacles and caring for people with dementia.
PWD cognitive and behavioural limitations
Physically getting PWD ready (such as bathing and clothing) was often difficult, according to caregivers. The procedure was described as “a tremendous production” and “a lot.” The approach was complicated by PWD’s old age and comorbidities, necessitating alterations to the morning schedule on the day of the visit.
For more info check out (Source):
